 In the final days of the rush to comply with the much-anticipated GDPR legislation ahead of the 25th May deadline, we discovered a ‘soft opt-in’ ICO clause.
In the final days of the rush to comply with the much-anticipated GDPR legislation ahead of the 25th May deadline, we discovered a ‘soft opt-in’ ICO clause.
In plain English, this clause says is that if you give me verbal approval (during a Consultation, say) for me to send you my newsletter – in which there is always an ‘unsubscribe’ option – then your actual ‘opt-in’ written permission is not required after all, which is a great relief to everyone!
The actual wording – and this is taken from Page 2 of the GDPR Advice Sheet: Communicating with Patients (©Technology Tamed Limited 2018) headed ‘Marketing to Existing Patients’ – is:
‘The ICO has produced some specific guidance on communicating with existing “customers”, confirming that in most cases you do NOT have to contact your existing patients before May 25th to obtain their explicit permission to continue communicating with them.
This is what the ICO says: “131. Although organisations can generally only send marketing texts or emails with specific consent, there is an exception to this rule for existing customers, known as the ‘soft opt-in’. This means organisations can send marketing texts or emails if: · they have obtained the contact details in the course of a sale (or negotiations for a sale) of a product or service to that person; · they are only marketing their own similar products or services; and · they gave the person a simple opportunity to refuse or opt out of the marketing, both when first collecting the details and in every message after that.” *
Although this is not mentioned specifically in the GDPR Regulation text the ICO has confirmed that soft opt-in is permitted under GDPR. This means you may continue to email or text existing patients to tell them about new goods and services such as new therapists joining your practice as this would be deemed to be soft opt-in.
Note that you must provide a simple method for your patient to opt-out of receiving further marketing communications. This means having a clear option to unsubscribe from marketing emails (which is easy to do if you use a program such as Mailchimp) and in text messages giving the option for the patient to reply using a term such as “STOP” to remove them from the marketing database.’
You may remember that the ICO is short for the Information Commissioner’s Office, an independent authority set up to uphold information rights in the public interest, promoting openness by public bodies and data privacy for individuals.
I hope that’s clear for everyone and that we can now all move forward in the knowledge that we are all compliant!
* Source: https://ico.org.uk/media/for-organisations/documents/1555/direct-marketing-guidance.pdf





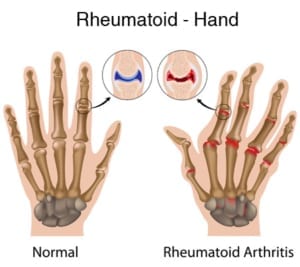
 The push for Evidence Based Medicine seems to be a double edged sword – without a double blind trial supporting a claim of efficacy, as required by The Advertising Standards Authority (ASA), one is unable to make claims for a treatment of any condition a patient may be suffering. With costly research, Osteopathy is lagging behind the ‘firepower’ of well-funded pharmaceutical companies.
The push for Evidence Based Medicine seems to be a double edged sword – without a double blind trial supporting a claim of efficacy, as required by The Advertising Standards Authority (ASA), one is unable to make claims for a treatment of any condition a patient may be suffering. With costly research, Osteopathy is lagging behind the ‘firepower’ of well-funded pharmaceutical companies. You may remember that I recently wrote about the BBC programme The Doctor Who Gave Up Drugs. Along similar lines I recently attended a workshop based on Cure: A Journey Into the Science of Mind over Body which is a bestselling book by Jo Marchant.
You may remember that I recently wrote about the BBC programme The Doctor Who Gave Up Drugs. Along similar lines I recently attended a workshop based on Cure: A Journey Into the Science of Mind over Body which is a bestselling book by Jo Marchant. Episode one is the first of a two-part social experiment in which Doctor Chris van Tulleken takes over part of a GP surgery and stops patients’ prescription pills. Here is a link to the program, which can be found on BBC iPlayer:
Episode one is the first of a two-part social experiment in which Doctor Chris van Tulleken takes over part of a GP surgery and stops patients’ prescription pills. Here is a link to the program, which can be found on BBC iPlayer:  Twenty years later, Doctor Tulleken’s fascinating two-part program illustrates how people suffering with, what he would describe as lifestyle illnesses can gradually begin to be weaned off their medication (with their GPs guidance); these patients suffer from a variety of different conditions including long-term chronic lower back pain, depression and hypertension, to name a few.
Twenty years later, Doctor Tulleken’s fascinating two-part program illustrates how people suffering with, what he would describe as lifestyle illnesses can gradually begin to be weaned off their medication (with their GPs guidance); these patients suffer from a variety of different conditions including long-term chronic lower back pain, depression and hypertension, to name a few.![sciatica_diagram [Converted]](https://www.robinkiashek.co.uk/wp-content/uploads/2018/12/sciatica_diagram-Converted-251x300.jpg)
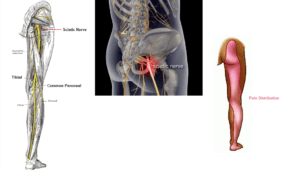 Here at the Robin Kiashek Clinics we promote prevention, and have plenty of advice on keeping your spine healthy and pain-free (
Here at the Robin Kiashek Clinics we promote prevention, and have plenty of advice on keeping your spine healthy and pain-free (