Travel tips for staying active (and pain-free) on holiday
Did you know, 27% of holidaymakers have either had or witnessed a travel partner have an accident on vacation?
That’s according to a 2024 survey* that found 35.88% of all accidents on holiday occurred from slipping, tripping or falling while on an excursion. While a further 31.18% of accidents on holiday were put down to slipping, tripping or falling in a hotel, due to wet floors or misplaced objects.
As an Osteopath with more than 30 years’ experience in the industry, I’ve seen all too clearly that unforeseen events can happen both in and out of the office. Whether it’s losing control while skiing, slipping on wet floor tiles around the pool or losing your footing and taking a tumble due to uneven ground.
But it’s how one confronts and deals with these sudden surprises — both physically and/or emotionally — that’s important.
Cycling Accidents Happen
For example, just this month, while taking some time away from my North London clinic, I ventured out on a bike ride.
Cycling is something I’ve been doing for years. But while out, enjoying the early signs of spring, I miscalculated a kerb and came toppling off my bike. This resulted in a painful sprain, a very nasty scrape along one side of my body and a slightly wounded sense of pride.
As I’ve written about previously, I like to see the glass half full not half empty. So the positive spin on this is that two very nice passers-by very quickly came over to help. While another pedestrian offered to usher me into their nearby office so I could receive first aid.
Lessons in Ageing Gracefully: Travel Safely and Stay Strong
As you age, there is a tendency to get stuck in one’s old ways. But this ‘banana skin’ moment of mine brought to mind one of my favourite phrases — that being: one’s greatest strength is one’s greatest weakness, and one’s greatest weakness is one’s greatest strength.
In this instance, what my body was able to do when I was 25 simply isn’t the case at 68. I’m a big believer in staying active and moving your body. But life is a series of calculated risks and if you win, you will be happy, if you lose, you will be wiser.
Therefore, if you are heading off to sunnier climes this month or beyond, it’s always worth pushing yourself. But, as this unforeseen event has reminded me, it’s even more important to know your limits. So, to help you stay active and injury-free on holiday, here are some top tips:
- Stay active. For some, a holiday is a chance to escape the daily grind and simply allow their minds and bodies to recharge. Of course, rest is important. But so is balance. Therefore, if you’ve got a long haul flight, stretch your legs by walking up and down a few times and once you’ve reached your destination, remember to take a short break from sitting on your sunlounger every half hour.
- Bend at the hips and not your back. Try to do this by keeping your upper body upright as much as possible and your chest forward. Doing so can help prevent any mishaps that can come from lifting heavy items awkwardly, like heaving suitcases on and off the baggage carousel.
- Use a rucksack. During day trips carry your travel essentials in a well-fitted rucksack, using both straps, rather than flinging a bag over one shoulder.
- Ditch flip-flops. Instead, invest in a good pair of walking shoes. Doing so will cushion your feet, support your soles and help with shock absorption. And, if you are planning on heading out on a run, I’d recommend going to a specialist running shoe shop to get fitted.
- Consider your posture. Yes, even on holiday as tech neck, from staring down at your phone, doesn’t just arise at work. If you can, sit up straight, don’t slump chairs and walk with your shoulders back and head up (not staring at the ground).
How Osteopathy can help
The human body has the innate ability to heal given half the chance. And in my time as an Osteopath, I have used many non-invasive methods, like gentle osteopathic techniques, to help to increase the mobility of the joints and relieve muscle tension.
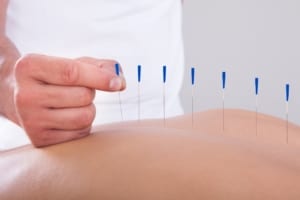
I have also trained in various additional complementary disciplines including Western Acupuncture — which can help to enhance the blood supply to the tissues, which in turn promotes the body’s natural healing process — and Low Level Laser Therapy — which can stimulate your cells to repair tissue and reduce inflammation and pain.
Ready to Feel Better? Get in Touch with Osteopath Robin Kiashek Today
Osteopath Robin Kiashek is registered with both the The General Osteopathic Council and The British Naturopathic Association, and is committed to helping his patients achieve physical and emotional wellbeing. Whether you’re dealing with pain or injury at home or abroad, Robin offers personalised care to help you recover and thrive.
Get in touch. To book a consultation, please click here.